Head pain that centers around the forehead, eyes, cheeks, or jaw can be frustratingly hard to decode. Many people assume it’s “sinus” related—especially when pressure builds behind the eyes or along the cheekbones. But a large share of recurring “sinus headaches” are actually migraine (or migraine-spectrum headaches), and treating the wrong problem can mean months or years of unnecessary symptoms.
This article explains how migraine can mimic sinus issues, common facial triggers, red flags that require medical attention, and where treatments range from lifestyle strategies to prescription options. We’ll also cover an evidence-based therapy that surprises many readers: Botox, which can help some people with chronic migraine.
Why migraine is often mistaken for a sinus problem
Migraine isn’t “just a bad headache.” It’s a neurological condition that can cause a collection of symptoms—many of which involve the face:
pressure or pain around the eyes and cheeks
nasal congestion or a runny nose
watery eyes
sensitivity to light, sound, and smells
nausea or appetite changes
scalp tenderness
fatigue and brain fog before or after the pain
Because congestion and facial pressure can occur during migraine, people may assume they have recurrent sinus infections—especially if the pain feels like it sits “in the face.” The clue is pattern and recurrence: true bacterial sinus infections are less common and usually come with signs of infection that persist.
Quick distinction: migraine-like vs infection-like features
More consistent with migraine:
recurring attacks with similar patterns
sensitivity to light/sound, nausea
symptoms triggered by sleep disruption, stress shifts, certain foods, hormones
facial pressure without high fever
More consistent with a sinus infection:
thick discolored nasal discharge with persistent symptoms
fever
symptoms lasting beyond the typical course of a viral cold
worsening after initial improvement (“double sickening”)
This doesn’t replace a clinician’s diagnosis—but it can help guide the right next step.
Common migraine triggers that affect the face and jaw
Triggers vary widely person to person, but these are commonly reported:
Sleep changes (too little, too much, or irregular schedule)
Stress swings (including “let-down” migraines after a busy period)
Hormonal shifts (especially around menstruation)
Dehydration and missed meals
Alcohol (often red wine for some people)
Strong smells and bright or flickering light
Weather changes (barometric shifts)
Neck tension and posture strain
Jaw clenching / bruxism (can overlap with headache disorders)
It’s also common for symptoms to stack: a late night + dehydration + skipped lunch can be the perfect storm.
Red flags: when to seek urgent medical care
Most headaches aren’t dangerous—but some symptoms should be assessed promptly:
a sudden “worst headache of your life”
new neurological symptoms (weakness, slurred speech, confusion)
headache after head injury
fever with stiff neck or rash
new headache pattern after age 50
headaches that are progressively worsening over weeks
persistent vision changes
If any of these apply, don’t self-diagnose—seek medical help.
The foundation: strategies that reduce migraine frequency
Many migraine plans start with reducing the “baseline vulnerability” so your threshold is higher.
1) Protect sleep consistency
A stable bedtime/wake time—especially on weekends—often helps more than people expect.
2) Hydration + regular meals
Dehydration and blood sugar dips are common triggers. A simple habit is pairing caffeine with water and adding a protein-forward breakfast.
3) Track patterns, not perfection
A short symptom diary can reveal high-impact triggers (sleep, alcohol timing, screen exposure, cycle-related patterns) without obsessing over every detail.
4) Manage neck and shoulder tension
Gentle mobility, ergonomic changes, and targeted strengthening can reduce musculoskeletal contributions that “feed” headache cycles in some individuals.
5) Avoid medication overuse
Overusing certain pain relievers can create rebound headaches in some people. If you’re taking acute medication frequently, it’s worth discussing with a clinician.
Treatment options: acute vs preventive
Migraine care often includes:
Acute treatments: taken at the start of an attack to reduce severity/duration
Preventive treatments: taken regularly to reduce frequency and intensity over time
Preventive therapy is usually considered when attacks are frequent, disabling, or not responding well to acute strategies.
Where Botox fits: a proven option for chronic migraine
Botox (botulinum toxin) is widely known cosmetically, but it also has a legitimate medical role in neurology. The key detail: Botox is used for chronic migraine, not occasional headaches.
What “chronic migraine” means
In clinical practice, chronic migraine is typically defined as:
headaches on 15 or more days per month, with a significant portion having migraine features, for at least 3 months
If someone has migraines a few times a month, Botox is usually not the first choice. But for chronic migraine, it can be an important option.
How Botox helps migraine (in simple terms)
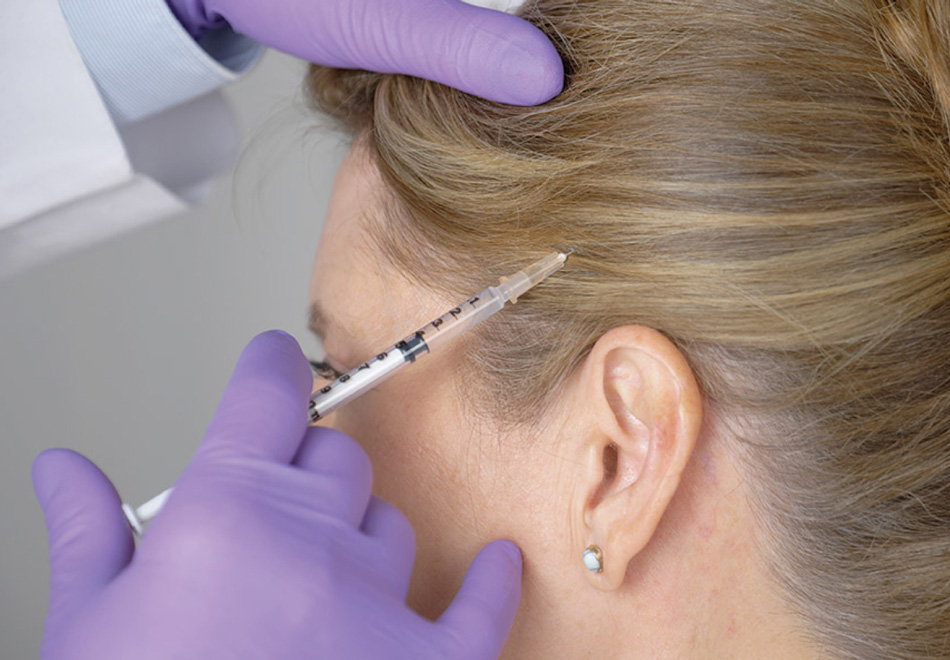
Botox is thought to reduce migraine frequency by affecting pain pathways and nerve signaling involved in migraine—not by “masking” pain. Treatment is done via a standardized set of small injections in specific areas (commonly across the forehead, temples, back of head, neck, and shoulders).
What to expect
Treatments are typically repeated about every 12 weeks.
Many people need more than one cycle to judge effectiveness.
The goal is usually fewer headache days, lower intensity, and better function—not necessarily zero headaches.
Side effects and limitations
Possible side effects can include temporary neck soreness, injection-site discomfort, mild weakness in nearby muscles, or eyebrow/eyelid heaviness in some cases. Botox should be performed by an appropriately trained clinician following migraine protocols—not purely cosmetic patterns—when the goal is migraine prevention.
Migraine vs “tension” vs TMJ: overlaps are common
People can have more than one headache contributor at the same time:
migraine plus neck strain
migraine plus jaw clenching
migraine plus poor sleep
That’s why a multi-pronged approach often works best—especially when facial pressure, jaw tightness, and forehead pain overlap.
